Why Breast Milk?
It’s a well known fact that the best nutrition for a newborn baby is breast milk; but for a premature baby it is particularly important as it contains antibodies from the mother which helps a baby’s underdeveloped immune system. As a premature baby will have missed out on the time where their immune system is developing in utero, breast milk is one way of giving it a kick-start. Another argument for breast milk is the disease called Nectrotising Enterocolitis (NEC) that can occur in preterm babies, particularly those of less than 30 weeks gestation; this is a potentially fatal inflammation of the underdeveloped gut wall and lining. Breast milk helps to line the gut and reduce the risk of developing NEC, in fact Unicef research indicates that NEC is “20 times more common if the baby had received no breastmilk“.
Expressing
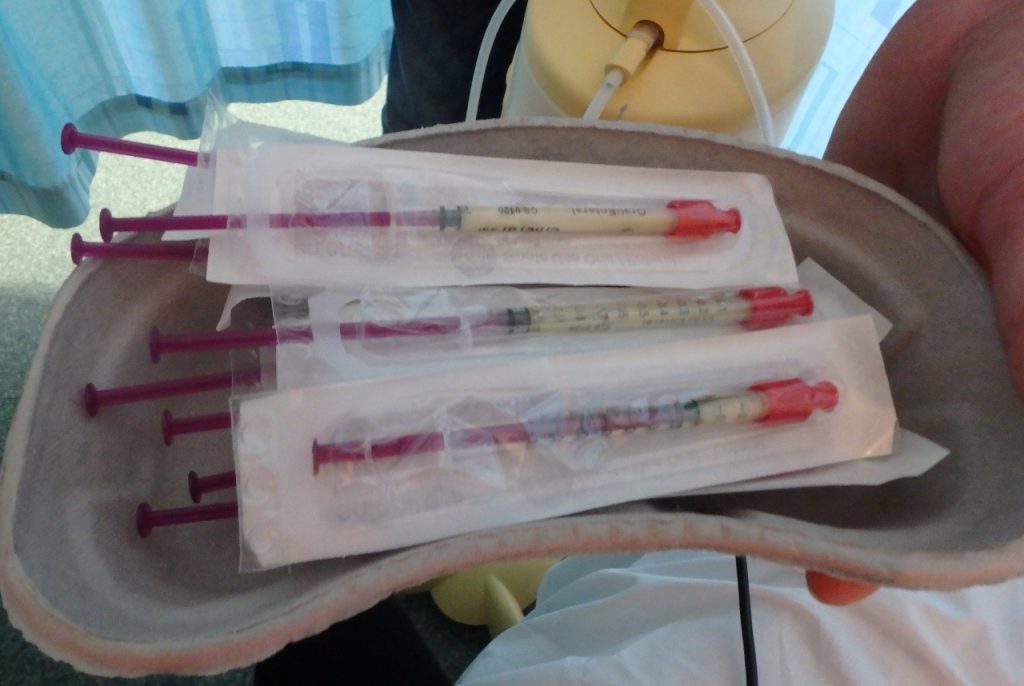
Expressed colostrum on day 2
So we know the reasons for breastfeeding but the actual act of breastfeeding is usually not possible at first with preemie babies who are likely to be tube fed for some time, depending on gestation (the suck, swallow, breathe reflex does not kick in until around 34 weeks gestation). This can make life quite difficult as not only are you dealing with the stress of having a premature baby but you now have something else to worry about, expressing milk. You can usually express next to your baby which minimises the amount of time spent away from them and for most of us helps milk supply too and proves to be a nicer view than the four walls of the pump room!
I was lucky in that I received some good advice on getting started with regards to expressing, the midwives on the ward told me not to use a breast pump for the first 24 hours after giving birth; instead it is best to hand express for this time. They showed me how to get started by demonstrating on a fake breast and immediately I set to work painstakingly hand expressing tiny droplets of milk into syringes. On these first few attempts just a small amount comes out but it’s important to remember where breast milk is concerned every little helps no matter how small, especially when it is the early milk called colostrum, also known as “liquid gold” as it contains a high number of antibodies to help fight infections and build a baby’s immune system. After the first 24 hours I was able to use a breast pump which made life easier and resulted in more milk as I found hand expressing made both my hands and breasts ache.
The main key to successful expressing is consistency; as tedious as it may be you do need to connect yourself to the breast pump every three to four hours and pump for ten to fifteen minutes or until the milk stops flowing, whichever comes first, even during the night. I did find night time expressing difficult but just kept telling myself that I would be up a lot more during the night if I had a baby at home.
Despite the best of intentions, sometimes the stress of the situation can take its toll and affect milk supply, which then snowballs as the lack of milk makes mums feel more stressed as they are then worrying about their babies being fed, this is perfectly normal too and if you are struggling with your milk supply despite following all the advice given, speak to your GP as medication called Domperidome can be prescribed to help, and speaking to other mums, for most it works really well..
Another remedy that worked well for a friend of mine, and from reading online is quite popular, is Jungle Juice. Here is an article that explains further and includes the recipe.
There are also some useful videos available from Unicef on expressing that you may find useful.
Successful Breastfeeding
I managed to leave the hospital exclusively breastfeeding Henry, something I was determined to do from the beginning so to make sure this happened I followed every piece of advice given to me along the way and asked as many nurses as possible for advice on the subject, especially those who had children of their own and had successfully breastfed themselves. To ensure our plan came together this is what worked for us:
- Once Henry was no longer ventilated we started using breast milk instead of water for mouth cares and started non-nutritive sucking with a pacifier dipped in breast milk when he received tube feeds so he would associate the sucking action and the taste with feeling full.
- Started non-nutritive sucking at the breast as soon as Henry was on Vapotherm at nearly 32 weeks. This means Henry was put to an empty breast after expressing just to get him used to sucking (it turns out he was quite good at it after all his preparation though so we had to stop until he was 34 weeks just in case he got a mouthful of milk and choked on it)
- At 35 weeks I attempted my first breastfeeding session, which went really well. Once we’d had a few days of successful feeds once a day we were encouraged to try two feeds per day, then three and finally four which is the maximum I could physically fit in during the time visiting.
- In the early days there were occasions when Henry was a little too sleepy; I was told to make him a bit less comfortable to wake him up, this included moving him away from my body a little and removing his blanket so he didn’t feel quite so snugly! Also techniques like tickling and stroking (and generally annoying him) were often affective in rousing him from his slumber. I then found that changing his nappy right before feeding was a sure-fire way to ensure he woke up and remained alert.
- As premature babies have very small mouths they may have some difficulty latching on, a great piece of advice that really helped Henry get started was to mould my breast into the right shape for his mouth, to do this cup your breast with your hand in a C-shape from underneath and squeeze gently, use the other hand to move the baby’s head forward and as soon as his mouth opens pop him on the nicely moulded breast. I know others have found nipple shields really helpful in supporting babies to latch on too.
- You may find your baby has a preference for one side. For quite a while I could not get Henry to feed from the left-hand side until a nurse suggested a rugby hold so he was held in the same position as he was on the right, in essence this tricked him into thinking he was feeding from the right. This worked most of the time really well, there was only the odd occasion where he would clamp his mouth tight forcing me to allow him to feed from his favourite breast! Now he happily alternates each feed and doesn’t need the rugby hold any more.
By the time we came to rooming-in Henry was a pro and luckily had no problem with adding night-time feeds into the mix. Since coming home, he is on a cross between three hourly and demand feeding, usually this is around three hours but sometimes less during a growth spurt (or when he’s just being greedy) or a little longer over night.
I must admit I was quite lucky with Henry, most babies still need top-ups when they first start breastfeeding but Henry likes to pig out! He was given a top-up the first time but didn’t really need it and as a result looked rather full and uncomfortable for the rest of the afternoon!
Don’t be disheartened if you have followed all the advice and are still struggling, some babies take longer than others, the important thing is to try not to get frustrated, some feeds will go better than others, just accept that and try again at the next feed. Henry didn’t always play ball during his non-nutritive sessions and sometimes you just have to take a deep breath and be patient.
